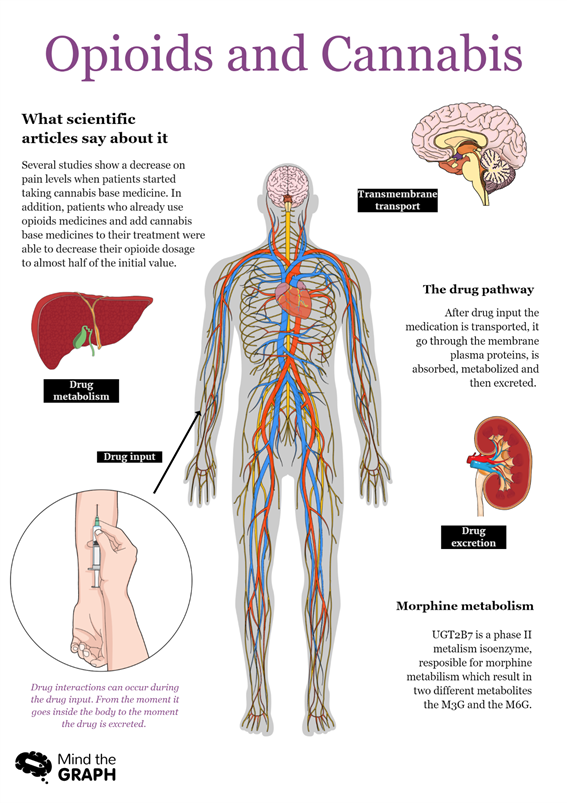
In the past decade many clinical trial studies reported positive and promising results in the use of cannabis-based medicines for neuropathic pain treatments.
Pain relief related to diabetes, chemotherapy, multiple sclerosis, fibromyalgia, osteoarthritis and several others have been treated with Cannabis.
Apparently, there is a connection between exogenous cannabinoids and opioids receptors, resulting in an increase in patient analgesia – the inability to feel pain.
Patients who are treated with opioids along with cannabis-based medications exhibit a medicament synergic effect, where the opioid efficacy is increased by the tetrahydrocannabinol – THC, the major psychoactive molecule in the cannabis plant.
Scientists are looking at these results with a positive perspective due to the possibility of a reduction in the opioids medication dosage, leading to a better quality of life to patients suffering from pain.
The endocannabinoid system, likewise other metabolic pathways is not an isolate system of the human body, it can influence and be influenced by other signaling pathways, one of these is apparently related to opioids and its receptors.
Opioids receptors besides the function of signalling sensation of pain, it also has the role to modulate some body functions like thermal regulation, hormonal stability, analgesic activity, among others.
Both, cannabinoids and opioids receptors are members of the G-protein-coupled family, which are proteins that have the capacity to influence neurotransmissions responsible for pain propagation in the brain and spinal cord.
The treatment of patients with chronic pain usually involves taking gradually increasing doses of opioids, which frequently lead to undesirable adverse side effects such as sedation, breathing disorders and constipation.
After a while, patients start to exhibit tolerance and resistance to the opioid dosage, not achieving its therapeutic effects, forcing doctors to increase the dosage repeatedly to achieve the same level of pain relief.
A high dose of THC alone is considered analgesic, but is usually followed by undesirable side effects like anxiety, headache, dry mouth, dizziness, euphoria and tachycardia, meanwhile, low doses do not produce analgesia effect at all.
Nevertheless, when combined with opioids this effect can be completely changed.
Studies conducted in animals’ models have shown that exogenous cannabinoids like THC can increase the efficacy of opioid medicines, like morphine.
The THC analgesic activity appears to be mediated through opioid receptors, having a cross-interaction between the cannabinoids and opioids signalling pathways.
Cannabis researchers report that THC administration can stimulate the production of endogenous opioids peptides in the body, which end up binding to already known opioids receptors – delta and kappa – intermediating the cannabinoid effect.
A third opioid receptor mu is also activated when morphine is administered. The activation of these three opioids receptors may be the explanation of the efficacy increase of the antinociceptive affect – the process of analgesia that blocks the detection of a painful stimulus – when compared to results of treatments of morphine or THC alone.
A study published in 2004 by Life Sciences journal confirmed the connection between THC and morphine by inhibiting opioid receptor using specific molecules.
The presence of blocking molecules resulted in a decrease of morphine efficiency, consecutively its therapeutic effects.
This result confirms how important is the availability of these receptors and its activation for morphine – and THC – treatment efficacy. Another experiment conducted with Naloxone – an opioid antagonist – blocked the THC activity in diverse regions of the brain, as ventral tegmental area, hypothalamus and periaqueductal gray (PAG), suggesting that these regions are somehow important to the interaction opioid-cannabinoid.
In addition, the study also reports that mice’s treatment with low doses of THC and morphine together did not lead to dosage opioid tolerance.
This study and many other are being published supporting the idea that cannabinoids when combined can increase opioids effect.
Cannabinoids apparently may also change the tolerance and addictiveness of opioids.
Long-term uses of opioids are usually associated with patients’ addiction, leading to the abuse of a substance that initially had only a therapeutic purpose.
Therefore, the combination cannabinoid-opioid – THC and morphine for example – could turn into a new analgesic strategy of combined therapy, allowing doctors to decrease high opioid doses of their patients and also decrease the level of opioid abuse and addiction of patients.
Besides, the theory of cannabinoids stimulating endogenous opioids, the detailed mechanism of the cannabinoid-opioid interaction system still remains unclear.
The hypothesis that tries to explain the potential mechanism of action is that cannabinoids maybe induce the synthesis or the release – of both – of opioid peptides, increasing the number of opioids receptors activated, resulting in the analgesic levels.
The elucidation of which peptides are involved in this process is not clear or known either, so, it would be crucial for scientists to fully understand the structure of these molecules and how cannabinoids can be used to produce analgesic effects, beyond assist in opioid addiction.
Howsoever, cannabinoids in general have been demonstrating surprising results, continually gaining space among medical professionals, proving its potential as an alternative medicine.
Several more studies are required for researchers to fully comprehend the real benefits and possibilities of cannabis-based medicines for the human body, and how is the best possible option to employ the cannabis plant as a treatment.
___
Did you like the infographic in this article? All icons used in this article – and many more – are available in the Mind the Graph. You can check the available illustrations in our gallery.
And you don’t need to start your infographic from scratch, we offer editable infographic templates to our users, so they don’t need to start from a blank canvas. Here you can see infographic templates.
You can also have a senior subscription and create unlimited figures, click here to start!
References
BROWN, J. D.; WINTERSTEIN, A. G. Potential Adverse Drug Events and Drug-Drug Interactions with Medical and Consumer Cannabidiol (CBD) Use. Journal of Clinical Medicine, v. 8, n. 7, 8 jul. 2019.
CICHEWICZ, D. L. Synergistic interactions between cannabinoid and opioid analgesics. Life Sciences, v. 74, n. 11, p. 1317–1324, 30 jan. 2004.
HANEY, M.; BISAGA, A.; FOLTIN, R. W. Interaction between naltrexone and oral THC in heavy marijuana smokers. Psychopharmacology, v. 166, n. 1, p. 77–85, 1 fev. 2003.
KUHLEN, M. et al. Effective treatment of spasticity using dronabinol in pediatric palliative care. European Journal of Paediatric Neurology, v. 20, n. 6, p. 898–903, 1 nov. 2016.
LÖTSCH, J. et al. Drug Interactions with Patient-Controlled Analgesia. Clinical Pharmacokinetics, v. 41, n. 1, p. 31–57, 1 jan. 2002.
LYNCH, M. E.; CLARK, A. J. Cannabis Reduces Opioid Dose in the Treatment of Chronic Non-Cancer Pain. Journal of Pain and Symptom Management, v. 25, n. 6, p. 496–498, 1 jun. 2003.
MANZANARES, J. et al. Pharmacological and biochemical interactions between opioids and cannabinoids. Trends in Pharmacological Sciences, v. 20, n. 7, p. 287–294, 1 jul. 1999.
WAKLEY, A. A.; CRAFT, R. M. THC−methadone and THC−naltrexone interactions on discrimination, antinociception, and locomotion in rats. Behavioural Pharmacology, v. 22, n. 5 and 6, p. 489–497, set. 2011.
WELCH, S. P. Interaction of the cannabinoid and opioid systems in the modulation of nociception. International Review of Psychiatry, v. 21, n. 2, p. 143–151, 1 jan. 2009.

Subscribe to our newsletter
Exclusive high quality content about effective visual
communication in science.