More than a half of the cases of dementia nowadays are classified as Alzheimer’s disease – a chronic neurodegenerative disease that gradually affects the cognition and memory of a person.
Until today it was thought to be caused by genetic and aging factors, the villains and key culprits of the illness are attributed to the senile plaques and the neurofibrillary tangled, leading to neuroinflammation and in sequence, neuron death.
However, a new theory of Alzheimer’s disease causes shines a light into the sky of medical research.
The theory is that genetics and aging are not the only factors responsible for the formation of amyloid clumps – the protein that accumulates between neurons causing Alzheimer’s disease – but it can be also a trigger response to microbe infection.
Let’s take a closer look at a neurological scale to understand the whole picture of what is happening inside a brain with Alzheimer’s disease. Two major phenomena are going on.
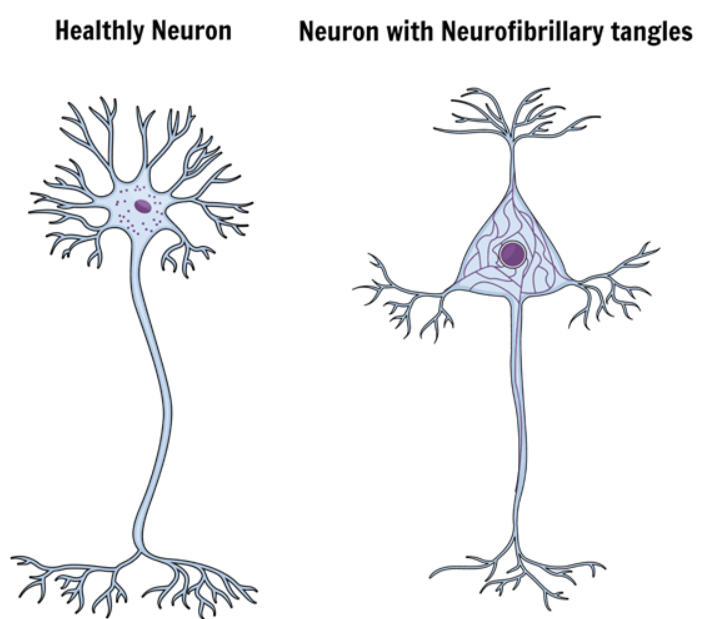
A protein called tau is responsible for maintaining stability by giving support to microtubules inside neurons. In a brain suffering from the condition, tau is biochemically modified by a reaction named hyperphosphorylate reaction.
The result of this change is insoluble proteins pieces inside the neuron, breaking down the whole system and killing neuron cells.
These insoluble pieces of tau proteins aggregate to each other forming the neurofibrillary tangles.
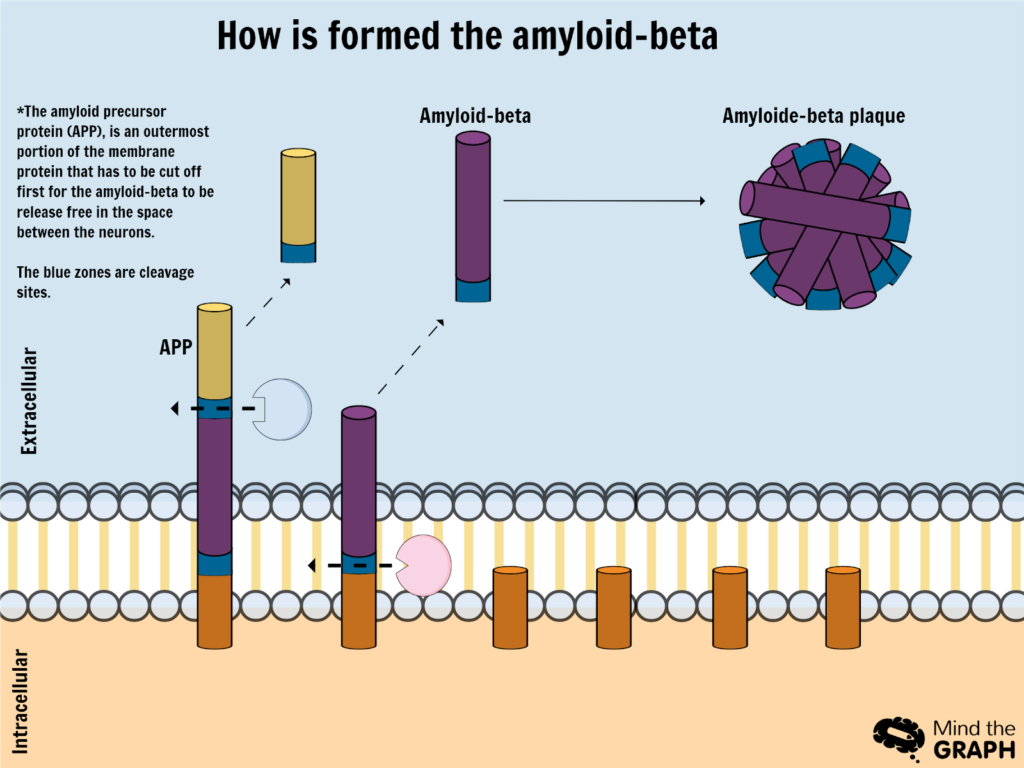
The senile plaques are made of amyloid-β peptides. A protein present in neurons membranes (pre-amyloid) suffers a cleaved process resulting into free pieces of amyloid-β outside the neurons*.
These pieces should supposedly be cleaned from the outer neuron medium by special cells and enzymes through phagocytosis, but because of genetic or aging factors, this process doesn’t happen efficiently enough, leading to free pieces of insoluble amyloid-β proteins that start to aggregate into plaques.
The amyloid plaques are the ones most studied and discussed to be the cause of Alzheimer’s disease. But scientist also affirm the neurofibrillary tangles is directly associated with the disease progression.
Scientists also found amyloid clump in healthy pos-mortem brains. Meaning that in a healthy old brain the cleaning process also becomes less efficiently, but not as much as a brain with Alzheimer’s disease.
Therefore, a large number of these senile plaques and neurofibrillary tangles are what characterizes the Alzheimer’s disease; they become extremely toxic to the brain and change the efficiency and quality of the synapses.
Subjects affected show symptoms like memory loss, confusion related to time and location, depression, anxiety, language and communication problems, mood instability, and others.
In the new proposed theory, the amyloid plaques are a mechanism of protection of the brain from microbe’s infection.
The amyloid-β gene is present in a big part of the vertebrate group and it has been preserved across different species for several generations, which means it should have a useful and important role to our body, not only acting as something harmful – if it wasn’t something valid or beneficial, the gene would be gone a long time ago through the evolutionary pathway.
Scientists went after thousands of post-mortem brains from people with Alzheimer’s disease.
Although they faced difficulties in analyzing these types of brain due to bad condition, they were able to study and collect information to later propose a few possible microbes’ triggers.
These triggers are mechanisms of defense against some types of human herpes viruses like herpesvirus 1, 6A, and 7, and three bacteria, Chlamydia pneumonia, Borrelia burgdorferi, Porphyromonas gingivalis.
The theory is that the beta-amyloid has initially a defensive function, trapping the microbes moving towards the brain, stopping a possible infection or disease.
As mentioned, due to factors of aging, the brain loses its capacity to effectively clean the amyloids. Thus, the idea of the amyloid function may be wrong all along; it is probably involved in a type of antimicrobial protection against brain invaders, being classified as an antimicrobial peptide.
Scientists have gotten positive results trying to demonstrate that β-amyloid could kill microorganisms from few common diseases.
In addition, another study that started in 2007 and is supposed to end in 2022 at the University of Columbia in New York is testing an antiviral drug in patients with herpes simplex virus 1 and mild Alzheimer’s disease, to see if the drug can slow down the progression of the disease.
For now, the only thing we can do is hope for the best and wait for the results.
This new proposed theory is still not well accepted by all scientific community. Many scientists argue that even if this new proposed theory comes to be proven, genetic factors and bad mutations are still going to be the main cause of the disease.
Alzheimer’s disease is still a condition with very little scientific knowledge of its real causes; there is no cure and not many therapeutic treatment options. If this theory ended to be true, it could be the first step in the direction of better treatments. Go science!
References
ABBOTT, A. Are infections seeding some cases of Alzheimer’s disease? Nature, v. 587, n. 7832, p. 22–25, 4 nov. 2020.
CECÍ, K. et al. Biomarkers in Alzheimer disease. Geriatrics, Gerontology and Aging, v. 6, n. 3, p. 273–282, 2012.
MAKIN, S. The amyloid hypothesis on trial. Nature, v. 559, n. 7715, p. S4–S7, 25 jul. 2018.
YOO, K.-Y.; PARK, S.-Y. Terpenoids as Potential Anti-Alzheimer’s Disease Therapeutics. Molecules, v. 17, n. 3, p. 3524–3538, mar. 2012.
___
If you need to create an infographic for scientific purposes – like me – in Mind the Graph you can create any kind of infographic you need and want. The platform is here to turn scientists into designers to increase their impact! Join us on the platform, click here!

Subscribe to our newsletter
Exclusive high quality content about effective visual
communication in science.